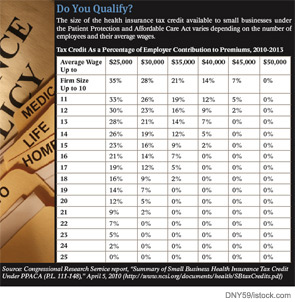
By now, you’re probably well versed in the clinical aspects of the health reform bill signed by President Obama in March. But what you may not know is that the bill includes a section that could benefit otolaryngologists and other physicians in their role as employers.