 Velopharyngeal insufficiency (VPI) causes significant quality of life issues for people affected—speech can sound hypernasal, as if too much air is coming out of the nose, and swallowing can send fluid back up through the nose, resulting in nasal regurgitation. A disorder in the velopharyngeal sphincter or valve that separates the nasal and oral cavities, VPI has a variety of etiologies.
Velopharyngeal insufficiency (VPI) causes significant quality of life issues for people affected—speech can sound hypernasal, as if too much air is coming out of the nose, and swallowing can send fluid back up through the nose, resulting in nasal regurgitation. A disorder in the velopharyngeal sphincter or valve that separates the nasal and oral cavities, VPI has a variety of etiologies.
Explore This Issue
April 2025In children, the most common causes are craniofacial abnormalities, including neuromuscular hypotonia and cleft palate (the most frequent cause of VPI in children). It also can occur in children after an adenoidectomy. In adults, the most common causes are degenerative neurological conditions and late effects or consequences of oropharyngeal and head and neck cancer treatments, including cranial neuropathies.
Correctly identifying the origin or cause of VPI is critical to successful treatment, which essentially involves closing the gap between the soft palate and the posterior wall of the throat. Surgery is a mainstay of treatment for more significant gaps, but physicians increasingly opt for a nonsurgical approach in select patients. In this procedure, called augmentation pharyngoplasty, injectable fillers are used to close the gap. Typically, this is used for small gaps, but it has been used successfully on medium gaps as well.
Shelagh Cofer, MD, a pediatric otolaryngologist at the Mayo Clinic in Rochester, Minn., who wrote her Triological Society Candidate Thesis on her results after using an injectable filler on children with VPI, is someone who has successfully closed small to medium gaps in both children and adults with VPI (Laryngoscope. doi.org/10.1002/lary.26227). She’s been using an off-label injectable dextranomer and hyaluronic acid copolymer (Dx/HA) since 2010 after looking for a more durable filler than other available fillers. She got the idea of trying the filler after noting that it had been used safely and effectively for years in the treatment of pediatric urinary reflux in Europe. Dx/HA is now also approved by the U.S. Food and Drug Administration. The product is commercially packaged as Deflux (Salix Pharmaceuticals, Inc., Raleigh, N.C.).
“This filler has a long track record in children, so almost 15 years ago, I started gingerly offering this to patients and developed a protocol for using it that a lot of people now follow,” she said. The protocol is available as a supplement to her thesis, as is a second appendix on how the procedure is performed.
The thesis described and reported on the results of a retrospective series of 50 children in which she used Dx/HA to fill small to medium gaps in the nasopharynx to treat VPI. She used the Golding–Kushner technique outlined by the International Working Group to estimate gap size (Cleft Palate Journal. doi.org/10.1597/1545-1569_1990_027_0337_sftron_2.3.co). It was the first series of patients to undergo augmentation pharyngoplasty with this new filler, and the results showed its benefits over traditional surgical approaches to correcting this problem: shorter procedural time to correct VPI, easier recovery, and, importantly, longer durability than reported with other types of fillers.
In 2017, Dr. Cofer and her colleagues also published a retrospective analysis on the efficacy and durability of Dx/HA in the treatment of 25 adult patients with VPI caused by neurologic etiology or benign anatomic etiology, or acquired following treatment for head and neck cancers (Mayo Clin Proc Innov Qual Outcomes. doi: 10.1016/j.mayocpiqo.2017.06.003).
In both the children and the adult series, Deflux has demonstrated longer durability to date than other fillers on the market. In the series on children, 80% of patients had a durable result at the end of one year, and 10-15% needed a touch-up injection. Of these latter patients, Dr. Cofer attributed the need for a touch-up to the change in pharynx volume that can be caused by a growth spurt in children and the potential need to open up the gap a bit. In 5% of the pediatric patients, the filler did not stay in the tissue. In the adult series, most patients (19 of 25) needed just one injection, and six patients needed a second injection.
I’m kind of a hole surgeon. If you have a big hole, you put something big in it; if you have a hole to the left, move everything to the left; if you have a tiny hole, you can do a lesser operation, and this is where I tend to use injectables for these tiny gaps. —Paul Willging, MD
Paul Willging, MD, a pediatric otolaryngologist in the division of pediatric otolaryngology–head and neck surgery and director of the Velopharyngeal Insufficiency Clinic at Cincinnati Children’s Hospital Medical Center in Ohio, is now also using Deflux in his patients, largely for small gaps. He was introduced to the idea by Dr. Cofer in 2010 when she came to Cincinnati to demonstrate its superior benefits over other fillers. Before that, Dr. Willging had tried several fillers that did not have the same durability as Deflux. He used medical-grade injectable Teflon in the early 1990s until it was no longer available; in the mid-1990s, he started using other fillers such as collagen products like Cymetra, often used for vocal cord paralysis, as well as calcium hydroxylapatite (Radiesse), often used for facial augmentation. Neither of these products proved to be a good long-term solution due to their relatively fast absorption (three to four months with Cymetra and six to 12 months with Radiesse).
Unlike Dr. Cofer, who has used Deflux in middle-sized gaps, Dr. Willging uses it only to close small gaps. “I’m kind of a hole surgeon,” he said. “If you have a big hole, you put something big in it; if you have a hole to the left, move everything to the left; if you have a tiny hole, you can do a lesser operation, and this is where I tend to use injectables for these tiny gaps.”
Dr. Willging determines the size of gaps with the “eyeball” approach when viewing the velopharyngeal sphincter area with a flexible endoscope. “If you see a tiny gap that looks like it is 2 mm in size and not extending all the way across, that is a gap I’ll inject,” he said.
Deflux has shown the longest durability to date compared to other common fillers used for VPI, but no head-to-head studies have been done, and the data is based on retrospective reviews of relatively small patient populations. Other fillers are still being used in this setting, and a sampling of how some laryngologists are using them is provided below.
Other Fillers Used
Jonathan M. Bock, MD, a professor in the division of laryngology and professional voice, department of otolaryngology and communication sciences, at the Medical College of Wisconsin in Milwaukee, mentioned several injectables, including hyaluronic acid (Restylane, Juvederm) for shorter-term temporary duration of six to 12 months, that may be suitable for augmenting Passavant’s ridge. He said if it is injected superficially, it can last longer. Another option for a longer-term duration is the use of autologous fat harvested directly from the patient via a small abdominal incision or liposuction technique and then injected directly into the posterior pharyngeal wall. A newer product that some physicians are trying is a silk protein microparticle–hyaluronic acid called Silk Voice. He cautioned, however, that both hyaluronic acid and Silk Voice carry the potential risk of allergic reaction and hypersensitivity.
Dr. Bock underscored the idea that the efficacy of these injectables is good as long as the palatal gap is not too large. “I generally try one to two injections with hyaluronic acid and, if beneficial, proceed to fat augmentation of the posterior pharynx in the operating room,” he said.
Noting that VPI has become a really huge issue in the quality of life of patients who have undergone nasopharyngeal and oropharyngeal cancer, Mark A. Fritz, MD, an associate professor in the division of laryngology, department of otolaryngology–head and neck surgery at the University of Kentucky College of Medicine in Lexington, said that filler injections for VPI have improved their quality of life.
For example, he noted that some patients have trouble swallowing after cancer treatment and, despite being treated for their esophageal stricture, are still so fearful of nasal regurgitation that it limits their willingness to go out to eat in public. They are afraid that something they swallow will come through their nose at the table. To correct this, he uses carboxymethylcellulose as a temporary injection to the posterior oropharyngeal wall and the soft palate that lasts two to three months, similar to its use in vocal fold injection augmentation. “If they get improvement with this temporary injection, oftentimes done concomitantly with another procedure such as vocal fold injection or esophageal dilation, then I will move towards doing an autologous fat injection augmentation again in the operating room as a way to get more permanent improvement,” he said.
Paul C. Bryson, MD, MBA, an associate professor of otolaryngology–head and neck surgery and head of the section of laryngology, department of otolaryngology–head and neck surgery at the Cleveland Clinic in Ohio, sees a lot of patients in his practice with late effects of head and neck cancer treatment and neurodegenerative conditions that cause VPI. He said injections are the predominant way he treats VPI. “There are surgeries, but often patient preference is for less intense treatment,” he said. “In addition, sometimes in a setting of prior surgery and radiation, the tissue healing and flexibility in this area is harder to predict.”
For Dr. Bryson, a key issue to keep in mind is the broad heterogeneity of VPI in patients, including gap size, tissue integrity, and symptoms. “I am careful to tell patients that this is definitely not a one-size-fits-all approach,” he said. “There are patients for whom it is hard to get a full response or to completely eradicate VPI with an injection. There is nuance and diversity in what you’ll see, and it is good to be aware of the ladder of options for patients.”
Best Practices
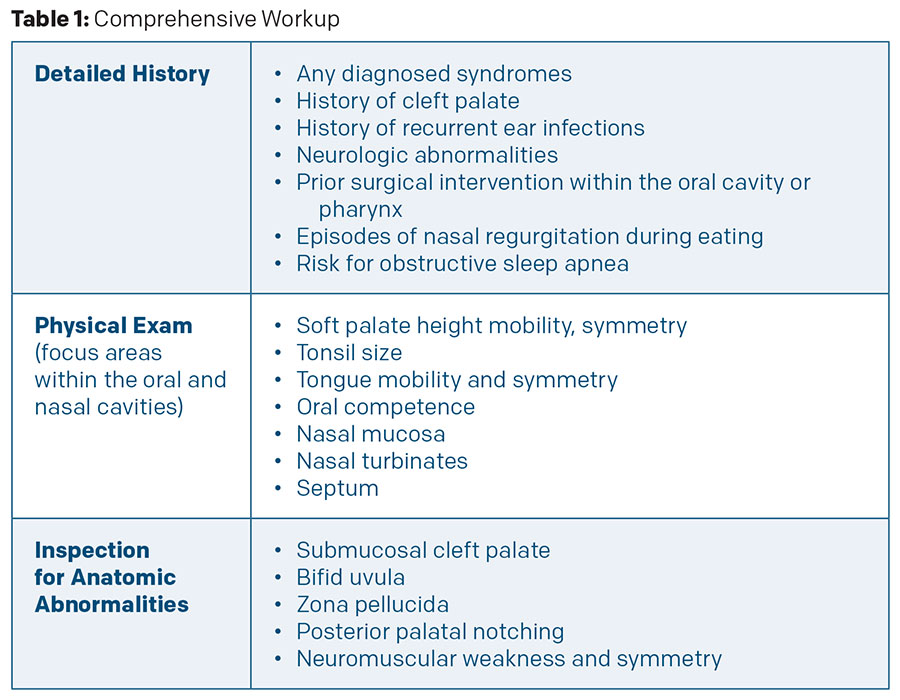
Patient selection is key to whether or not to use injectable fillers for VPI. To determine which patients meet the criteria for VPI, a thorough workup should be performed to determine the etiology of the VPI and the symptoms caused. This includes involving an interdisciplinary team of otolaryngologists, speech pathologists, and radiologists in conducting a thorough history, physical exam, assessment of speech production, and instrumentation evaluation (Table 1) (StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK563149/). A speech pathologist provides the gold standard for VPI diagnosis by asking patients to produce sounds to assess for hypernasal speech, misarticulation, or compensatory facial grimacing.
 Key takeaways to consider if you’re planning to use injectables for VPI:
Key takeaways to consider if you’re planning to use injectables for VPI:
Dr. Cofer
- Great option for patients who may not medically be able to undergo a major surgery;
- Great option for those with small to moderate gap size; and
- Essential that patients be treated by a physician/center with experience in using injectables in this setting.
Dr. Willging
- When using Deflux, there is a chance of the needle hub disconnecting from the syringe. He transfers the Deflux to a 1 ml TB slip tip syringe and then places it into a Bruning syringe. This prevents the potential loss of the material during the injection.
- Using the injectable correctly is critical. Generally, only inject it superficially into the submucosa.
- He uses prophylactic antibiotics in kids due to the insertion of the needle into a nonsterile site.
Dr. Bock
- Inject that material superficially.
- If not injected superficially, spinal infections may occur. To avoid this, many practitioners recommend the use of empiric antibiotic treatment.
Dr. Fritz
- Injection should be performed where the palate meets the posterior oropharyngeal wall to close the gap where this mobile structure will hit.
- To increase the amount of filler injected into irradiated tissue where there is no potential space in the posterior wall, he injects the filler into the soft palate itself with good effectiveness.
- Screen patients with neurologic issues or a history of head and neck cancer for VPI.
Dr. Bryson
- The patient population for VPI is heterogeneous.
- Detection and identification of VPI, along with patient symptoms, are the first steps to a treatment pathway.
For patients who are considered good candidates for injectable fillers, the size of the gap to fill is critical, with most experts interviewed for this article citing the use of injectables only for small sizes and most saying that there is no standard way of determining gap size. Dr. Cofer uses the standard cited in her article, the Golding–Kushner technique outlined by the International Working Group. In that scale, small gaps are less than 20% of the resting velopharynx, moderate gap sizes are 20%-50%, and large gap sizes are more than 50%. All the physicians interviewed for this article agreed that large gap sizes are not suitable for injectables.
Mary Beth Nierengarten is a freelance medical writer based in Minnesota.
Leave a Reply